Penile cancer
What is penile cancer?
Penile cancer is a type of cancer affecting the foreskin, shaft, or glans (head) of the penis. It is very rare, with only about 100 Australians receiving a diagnosis each year. Most cases occur in older men with a history of smoking.
There are many types of penile cancer, though over 95% of cases are squamous-cell skin cancers which develop on the penis. Penile sarcomas, which affects the deeper tissues, are more dangerous, and affect only about five men each year.
Sandhurst Urology offers diagnosis, management, and medical intervention for penile cancer from our clinic in Bendigo. To book an appointment, please ask your GP for a referral or call us directly.
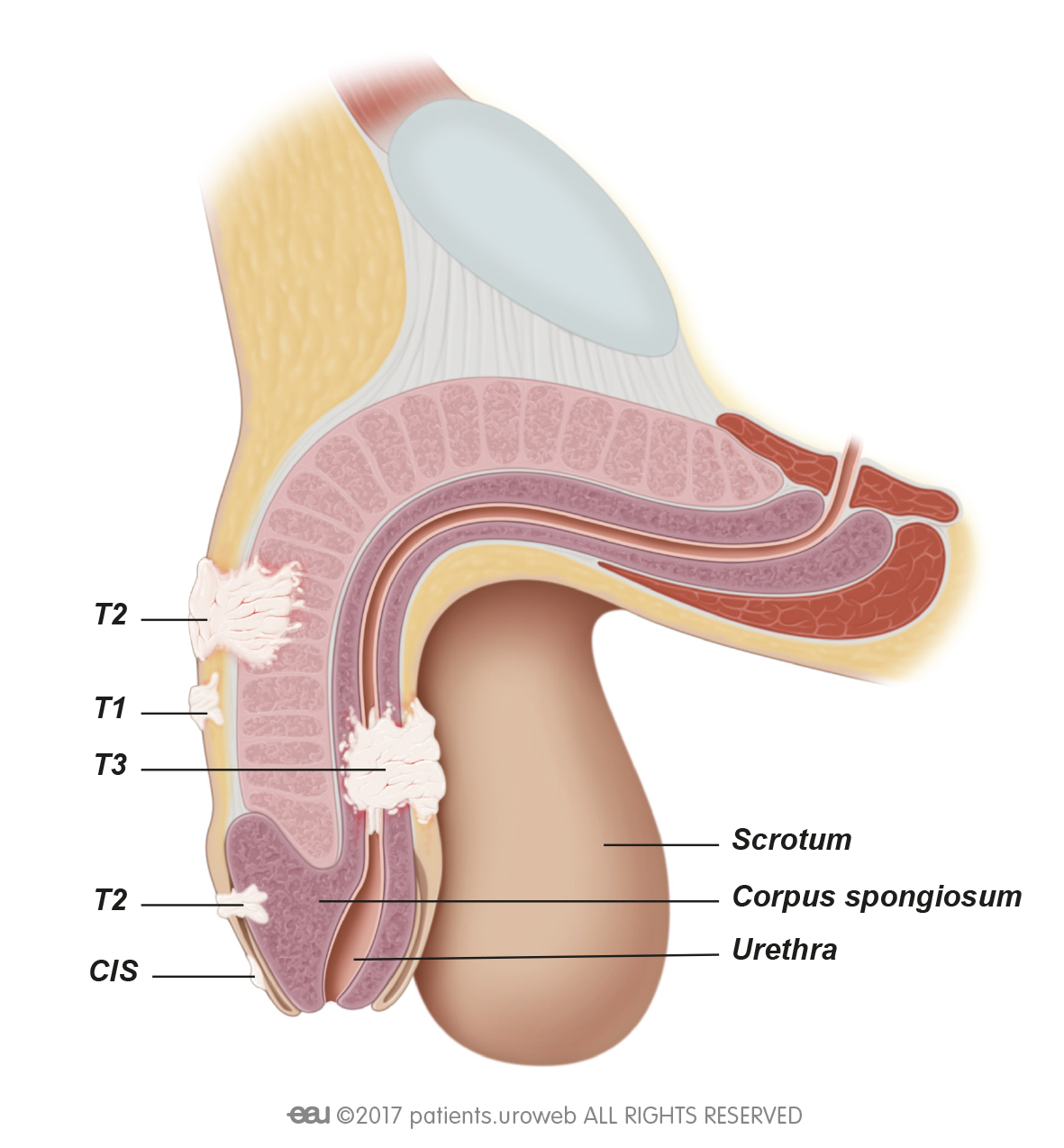

Symptoms
Symptoms of penile cancer may include:
- Blisters or sores on the penis which do not heal within a few weeks
- Hard lumps on or under the foreskin
- Flat or wart-like growths which discharge blood or pus
- Bleeding or bloody discharge from the penis or under the foreskin
- Foul-smelling discharge
- Changes in the skin of the penis (feeling thicker or changing colour)
- Rashes or persistent red patches on the penis which do not go away
- Lumps or swollen lymph nodes in the groin
Note that these symptoms do not necessarily indicate penile cancer – they may be symptoms of STIs or other medical conditions. Your own experience with penile cancer is highly individual and you may experience different symptoms to those specified here. Speak to a penile cancer expert at Sandhurst Urology for full diagnosis and treatment.
How penile cancer is diagnosed
Your doctor will generally begin by asking about your medical history and conducting a physical exam of the penis. They may physically inspect the penis for abnormalities and ask about any discomfort or changes to your sexual function.
If they suspect penile cancer, your doctor will usually request further tests to confirm a diagnosis. These tests may include:
- Blood tests – these measure your red and white blood cell counts and check for chemicals produced by cancer cells. They may also check for STIs or other potential causes of your symptoms.
- STI testing – your doctor may recommend other tests for HIV, gonorrhoea, and other sexually transmitted infections which affect the penis. As you can have both penile cancer and an STI at the same time, this test can rule out other causes of your symptoms and inform your treatment options.
- Biopsy – this involves removing a small patch of skin from the penis, which is sent to a laboratory and analysed for signs of penile cancer. The process is usually similar to a skin cancer biopsy on any other part of your body. Your doctor may also request a fine-needle aspiration biopsy (FNA) or sentinel lymph node biopsy, which collect samples form deeper inside the penis.
- Ultrasound – using high-frequency sound waves, this test lets the doctor visualise the internal soft structures of the penis and check for abnormal shapes or lumps.
- MRI – this test uses magnetic waves to create detailed cross-section images of the body. It may be used to see if the penile cancer has spread to other parts of the body.
- CT and PET scans – Similar to an x-ray, a CT scan creates still images of the inside of your body. they may be performed after injecting a small amount of radioactive glucose into the body which can that can highlight cancer cells (PET scan).
Preventing penile cancer
While there are no guaranteed measures for preventing penile cancer, several risk factors are known to influence its appearance and managing these may reduce your risk of developing it. Strategies to do this include:
- Avoiding smoking – chemicals in tobacco can damage cells in the body, contributing to many cancers.
- Practice safe sex – while penile cancer is not transmissible, STIs such as the human papillomavirus (HPV) and HIV/AIDS may increase its likelihood of appearing. Avoiding these by using barrier contraception may reduce your penile cancer risks. Some types of HPV can also cause genital warts which look similar to penile cancer.
- Avoid UV light exposure – as most penile cancers are skin cancers, avoiding UV exposure from sunlight, UV lamps, and tanning beds may decrease your risk of developing it.
- Treatment of Ballanitis Xerotica Obliterans (BXO). This condition of the foreskin and/or glans penis carries a 10% risk of developing penile cancer if not treated.
- Consider circumcision – though not medically necessary or recommended in most cases, men who have tight foreskins which are difficult to pull back may benefit from a procedure to remove the foreskin. This improves the ability to clean secretions away from the head of the penis, which may otherwise build up and cause inflammation which contributes penile cancer.
- Get vaccinated for HPV – most men who contract HPV do not develop penile cancer, though most penile cancer cases occur alongside an HPV infection. Being vaccinated improves your body’s ability to remove the virus.
As with any condition, always seek medical guidance to prevent and treat penile cancer effectively. Ask your GP for a referral to Sandhurst Urology for individualised advice.
Treatments for penile cancer
Treatments for penile cancer aim to remove the cancer and prevent it from returning while avoiding damage to the penis as much as possible. Your treatment team will suggest options for doing this which are most likely to benefit you. They may include:
- Radiotherapy – this treatment uses high-energy rays to destroy cancer cells and minimise harm to surrounding healthy cells. It is not usually recommended to treat the primary penile cancer tumour, though it may be used to treat cancer which has spread to the lymph nodes.
- Chemotherapy – chemotherapy involves using medications designed to kill cancer cells. The type used to treat penile cancers is usually a cream which you can apply at home. More severe penile cancer cases may benefit from chemotherapy taken in tablet form or via injection.
- Circumcision – if your doctor prescribes a chemotherapy cream to treat your penile cancer, they may also recommend a small surgery to remove the foreskin. This allows both you and your doctor to effectively see and manage the cancer during treatment. Circumcision may also treat penile cancer fully of the cancer is localised to the foreskin.

Medical interventions for penile cancer
Treatments offered through Sandhurst Urology include the following:
- Local excision – penile cancers which are localised to the skin’s upper layers may be treated by removing the patch of skin containing them. Your doctor will usually remove some healthy tissue surrounding the cancer spot to prevent it from returning. Some local excisions need a small skin graft to heal properly, which is generally taken from your thigh and attached in the same procedure.
- Glans resurfacing – larger cancers that affect the head of the penis (the glans) may be treated by removing the top layer of skin (the mucosa) and replacing it with a skin graft from your thigh. This procedure usually does not damage sexual function and produces good cosmetic results.
- Glansectomy – larger cancers involving the head of the penis (glans) may be treated by removing the glans in its entirety. The surgeon will usually replace it with a layer of skin taken from the thigh to produce good cosmetic results. Glansectomy generally does not affect sexual function, though it may impact the penis’s sensitivity.
- Penectomy – this procedure removes penile cancer by removing part or all of the penis. It is generally recommended only if your penile cancer affects a large area or if other treatments have failed. If they need to recommend a penectomy, your doctor will usually discuss options to surgically reconstruct the penis.
Providing Excellent Urological Care of the Highest Standards
Book a consultation with Sandhurst Urology today